Glaucoma is a disease affecting the visual acuity i.e the ability to see. It is the second leading cause of blindness (after cataract) and the most significant cause of irreversible blindness globally. At present, 8 million people are bilaterally blind due to glaucoma. As per the estimate suggested by the International Agency for the Prevention of blindness, 80 million people will suffer from glaucoma by the year 2020.
It is necessary to understand the basic human eye anatomy in order to comprehend the pathophysiology involved in the disease. The human eye is a specialized visual organ which consists of a complex of structures. Iris is the colored part of the eye. Cornea is the dome covering the iris. Pupil is the black circular opening in the iris that lets the light in. Just behind the iris and the pupil lies the lens which helps focus light on the back of the eye. The inner lining of the eye contains special light-sensing cells known as retinal cells. When we see an object, the light passes through the pupil and lens to the back of the eye where retinal cells convert light into electrical impulses. These impulses are carried to the brain by the optic nerve. This is how the object is visualized and interpreted by the human eye. Glaucoma is characterized by the degeneration of the optic nerve, hence, causing impaired visual perception.
But what damages the optic nerve? The answer to this question lies in the concept of aqueous humor and Intraocular pressure (IOP). Aqueous humor is a clear fluid present in the front part of the eye which nourishes the structures within the eye. This fluid is constantly produced by the ciliary body, which surrounds the lens of the eye. The aqueous humor then passes through the pupil and leaves the eye through tiny drainage channels, scientifically termed as trabecular meshwork. These channels are located at something called as drainage angle of the eye (the angle where cornea attaches to the base of the iris). The adequate production and effective drainage of the aqueous humor is necessary to maintain the normal pressure within the eye, medically known as IOP. In glaucoma, there is elevated IOP which causes irreversible degeneration of optic nerve, hence, leading to visual impairment, which if left untreated can lead to blindness.
Types and Symptoms of Glaucoma
Types of Glaucoma:
Based on the underlying mechanism and patency of the drainage angle of the eye, glaucoma can be of several types.
- Open-angle Glaucoma: It is the most common form of glaucoma. As the name implies, the drainage angle remains open. But, there is a partial obstruction to the trabecular meshwork, thus, hindering the drainage of aqueous humor. This eventually results in raised IOP and optic nerve damage leading to glaucoma.
- Closed-angle Glaucoma: In this type, the iris bulges forward to obliterate the drainage angle contributing to elevated IOP caused by the build-up of aqueous humor.
- Normal-Tension Glaucoma: In this type of glaucoma, the IOP is within the normal range and glaucoma is caused by damage to optic nerve. The exact cause of this type of glaucoma is a matter of controversy for the researchers. It may be due to a sensitive optic nerve or due to impaired blood flow to the optic nerve. This impaired circulation can be due to atherosclerosis (build-up of cholesterol plaque in the arteries) or due to other conditions that impair circulation.
- Glaucoma in children: It is possible for an infant or a child to present with glaucoma at the time of birth or in initial years of life. It can occur due to obstruction in the drainage system of the aqueous humor or due to some underlying medical condition.
- Pigmentary Glaucoma: As already stated, iris is the colored part of the eye. It contains pigments which can get dislodged and block the drainage channels of the eye, thus causing raised IOP and eventually glaucoma. Rigorous activities such as running, etc can lead to such dislodgement and a transient state of raised IOP.
- Secondary Glaucoma: It results from an inflammation, injury or vascular disease causing an increased IOP. Trauma to the eye is a major cause of secondary glaucoma.
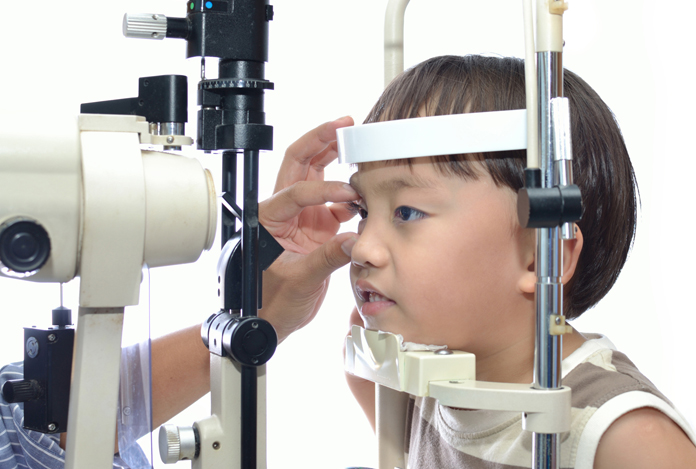
Symptoms of Glaucoma:
Glaucoma is often termed as “the sneak thief of sight” as it is usually indiscernible in the initial stages and is almost invariably diagnosed in late stages when it has progressed substantially to cause irreversible damage.
The patients with glaucoma are unable to see the objects within their particular field of vision or the visibility is limited. A point of significance is that initially there is loss of peripheral vision which is usually left unnoticed by the patient, thus making the disease progress to its final stage which is marked by loss of central vision too. There are appearances of blind spots which makes it difficult for an individual to lead a normal life. Activities such as driving become cumbersome as the individual is able to visualize the street ahead but finds it difficult to visualize the people walking on the sidewalks. People also complain of difficulty in adjusting to changes in light such as entering a dark room immediately after outdoors. People with glaucoma also finds it difficult to perceive obstacles such as steps, etc.
Evident clinical findings such as red eye are rare and can be seen in cases of secondary glaucoma caused by recent trauma to the eye. Occasionally, there may be a sudden rise in IOP leading to symptoms such as headache, pain in the eye and presence of halos around the eyes.
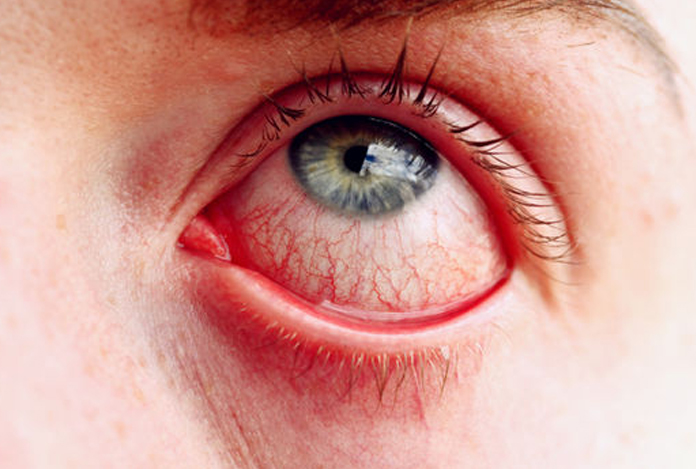
Risk Factors of Glaucoma
Although everyone is at risk of developing glaucoma, there are certain risk factors that predispose an individual to it. The significant risk factors are:
- High IOP: It is important to understand that not all individuals with high IOP show symptoms of glaucoma. However, it must be considered as a warning sign and appropriate treatment must be undertaken to avoid the consequences.
- Age: Individuals above 45 years of age are at a higher risk of developing glaucoma.
- Hereditary inheritance: Glaucoma has a hereditary predisposition. Thus, if you have a family history of glaucoma, it is important to get frequent eye examination by an ophthalmologist.
- Ethnic origin: Blacks are at a much higher risk than people of other ethnic origins.
- Certain medications: Use of steroids (systemic or topical), particularly as eye drops can predispose an individual to glaucoma.
- Co-morbidities: Presence of conditions such as diabetes, hypertension, cardiovascular diseases and sickle- cell anemia raises the risk of developing glaucoma.
Certain eye conditions such as nearsightedness and farsightedness also increase the risk of developing glaucoma.

Do I have Glaucoma?

If you are experiencing blurring of vision, have a recent history of trauma to the eye, can see blind spots in your field of vision or are unable to see peripheral objects, these along with a positive family history raises a strong suspicion of glaucoma and you must visit your eye doctor soon.
Causes and Prevention of Glaucoma
As described earlier, the most important cause of glaucoma is raised IOP which can be due to an abnormality in production or drainage of aqueous humor, or both. It may be impossible to prevent glaucoma, but steps can be taken to detect glaucoma at an early stage and hence, prevent its debilitating consequences.
- Know your family’s eye history: Prior knowledge of one’s family history can alert the individual and he/she should undergo regular eye check-ups.
- Get regular eye check-ups: Eyecare must not be underestimated and people must get their eyes checked frequently. Frequency depends on the age of the person and the genetic susceptibility. Eye check-ups should be undertaken every 4 years after age 40 and every 2 years after age 65. In case of high genetic risk, the frequency of check-ups should increase.
- Wear eye protection: When performing an activity with increased risk of trauma to the eye, appropriate protective wear must be worn to prevent any injury to the eye, hence, reducing the risk of developing secondary glaucoma.
- Keep your blood sugar in check: As we already know by now that diabetes increases the risk of glaucoma, hence it is essential to monitor your blood sugar levels timely and consult your physician to maintain a normal blood sugar level.
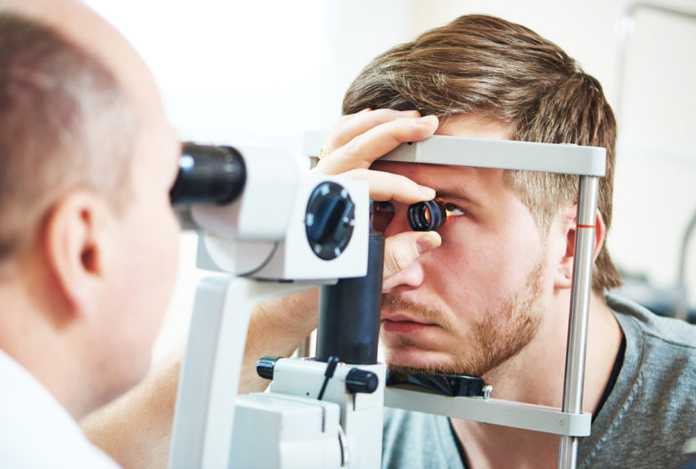
Diagnosis and Tests for Glaucoma
An eye specialist called as Ophthalmologist must be sought if suspecting visual disturbances.
An ophthalmologist can diagnose glaucoma even before it has shown its first symptom. The various diagnostic modalities used by an ophthalmologist are listed below.
- History of symptoms: A thorough history taking and appropriate investigations form the basis of diagnosis of glaucoma. History of the symptoms, particularly duration, presence or absence of blind spot and the extent of loss of visual field are assessed by the ophthalmologist.
- Ophthalmoscopy: Examination of the eye is the next step in the diagnosis. A special instrument, known as ophthalmoscope is used to see the eyes internally. It aids in checking if the optic nerve is damaged or not.
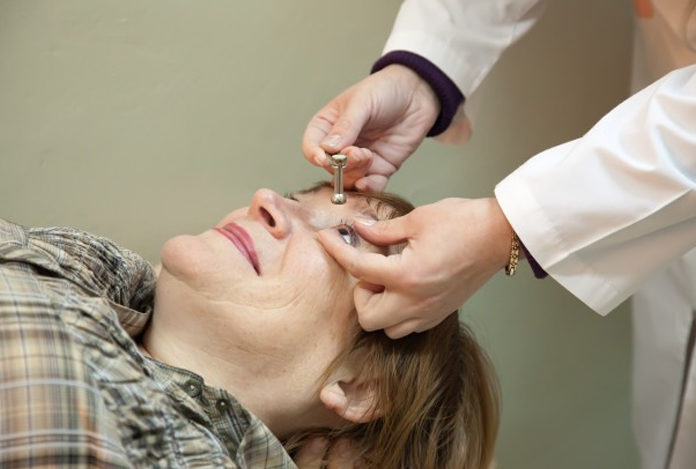
- Tonometry: Another important investigation carried out by an ophthalmologist is known as tonometry, wherein the eyes are rendered numb with an eyedrop and small tip of a measuring device is placed against cornea to check the intraocular pressure.
- Pachymetry: This procedure determines the thickness of cornea. It precedes tonometry as thick cornea can hamper the IOP findings. In this procedure, the eyes are made numb with an eyedrop and a pachymeter tip is used to measure the thickness of the cornea.
- Gonioscopy: It is done to assess the type of glaucoma. It involves numbing the eye and placing a special type of mirrored contact lenses onto the surface of the eye to look inside the eye and determine the drainage angle, whether it is open angle or closed angle.
- Confocal laser scanning systems and optical coherence tomography are non-invasive methods to achieve a 3-D image of the optic nerve and retina.
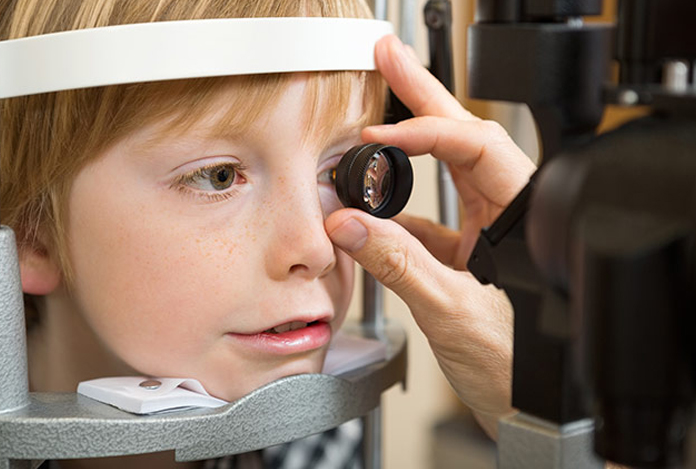
Treatment and Care of Glaucoma
Once the diagnostic workup is done, the ophthalmologist offers appropriate treatment to the individual.
Medications:
Various drugs have been advocated in the treatment of glaucoma.
Beta-adrenergic antagonists are administered as eye drops. This class of drug reduces the secretion of aqueous humor, thus normalizing the IOP. These include medications such as timolol, levobunolol, carteolol, and metipranolol.
But, due to some major cardiac side effects (reduced heart rate and low blood pressure), beta-adrenergic antagonists have been replaced with another class of drug known as prostaglandin analogue. This group of drug causes effective drainage of aqueous humor, thus relieving the raised IOP. Prostaglandin analogues include latanoprost, travoprost, bimatoprost, and tafluprost.
Another class of drug known as adrenergic agonists helps in glaucoma by both, reduction in production of aqueous humor and facilitating its effective drainage. The most popular adrenergic agonist is brimonidine.
Osmotic agents are another important group of drugs which are used in acute cases of glaucoma but must be used cautiously as they can cause major side effects such as nausea, fluid accumulation in heart and lungs, bleeding in the brain and kidney problems. Examples of osmotic agents include isosorbide (ismotic, administered orally) and mannitol (Osmitrol).
Laser:
There are various forms of laser therapy useful in the treatment of glaucoma.
Laser iridotomy is done in closed-angle glaucoma. In this procedure, a hole is made in the iris to drain out the excessive aqueous humor.
Laser trabeculoplasty is used as an adjuvant along with the medications. In this procedure, laser is applied through a mirrored contact lens in the corners of the eye causing minor laser burns in them, thus causing the drainage of fluid.
Laser cyclo-ablation is used when all other treatment modalities have failed to produce outcomes. In this procedure, the aqueous humor producing cells known as ciliary body are destroyed by laser application.
Glaucoma surgery:
In severe cases of glaucoma, surgical intervention might be needed.
Trabeculectomy is the most commonly used surgery and produces the most significant reduction in IOP. It involves removal of a small piece of the clogged trabecular meshwork in order to facilitate fluid drainage. A small collecting bag, medically termed as “filtering bleb” is created in the conjunctiva to collect the drained fluid and pass it on to the blood.
Aqueous shunt devices (glaucoma implants or tubes) involve the use of artificial devices such as a plastic tube inside the eye to drain the excess fluid and a plastic reservoir beneath the conjunctiva to collect the excess fluid.
However, it must be kept in mind that there is no cure for glaucoma as it causes an irreversible damage to the optic nerve. Hence, the goal of therapy is directed at arresting the damage and preventing blindness.

OTC and Self-Management Methods for Glaucoma
There are various over-the-counter medications available to treat glaucoma. Trade names of the commonly used medications are listed below.
Medicines that reduce the production of aqueous humor
- Beta-blockers such as Betagan, Timoptic, Ocupress
- Adrenergic agonists such as Alphagan and propine
- Hyperosmotics such as Osmitrol
Medicines that facilitate the drainage of fluid
- Prostaglandin analogues such as Xalatan, Travatan, Lumigan and Zioptan
- Adrenergic agonists such as Alphagan and Propine
Guide to take glaucoma medications
- Always take your medications on time and in recommended dosage. If need be, use a measured dose dispenser.
- Learn how to administer eye drops as most of the glaucoma medications are prescribed as eye drops.
- Make sure all your doctors know that you have glaucoma as the glaucoma medications can cause drug interactions with other medicines. For instance, in case of closed-angle glaucoma, you must avoid the medicines that dilate the pupil such as antihistamines and medicines used for treating motion sickness.
Natural Ways to Cure Glaucoma
Although allopathic modalities are the safest methods to combat glaucoma, there is no denying the importance of alternative medicine in the treatment of glaucoma.
Herbal remedies: Various herbal remedies have been used in the treatment of glaucoma.
- Ginkgo biloba is the most popular and effective herbal remedy which improves the blood circulation to the brain and hence, alleviates symptoms of glaucoma
- Cayenne pepper contains capsaicin which has potent anti-inflammatory properties and hence, can eliminate the obstruction in the draining channels of the eye fluid. It must be used in a diluted state to produce effective results.
- Bilberry extract works as an antioxidant for the eye and strengthens the capillary walls of the eyes.
- Another herbal remedy is a combination of equal amounts of coriander seeds and fennel seeds. Prepare the seeds, add brown sugar loaf to the mixture and grind it to create a powder. 10 grams of the powder should be taken daily to produce desirable results.
- Combination of carrot juice and spinach juice is also a beneficial home remedy
Good nutrition can play a vital role. Nutrients such as Vitamin E, C and A as well as fatty acids and minerals can help protect the optic nerve.
Lastly, regular exercise and yoga are also beneficial in glaucoma.

Health Tip by Experts
At this point, it is important to emphasize that the damage caused by glaucoma cannot be reversed. Hence, the health experts strongly recommend that awareness of glaucoma is necessary on a global level. Every individual must be aware of all the risk factors of glaucoma and must take preventive measures in order to facilitate early detection of glaucoma. People must realize that glaucoma is not just a disorder affecting the physical well-being of the individuals, but it also has major psychological implications associated with blindness, thus violating the independence of leading a normal healthy life.