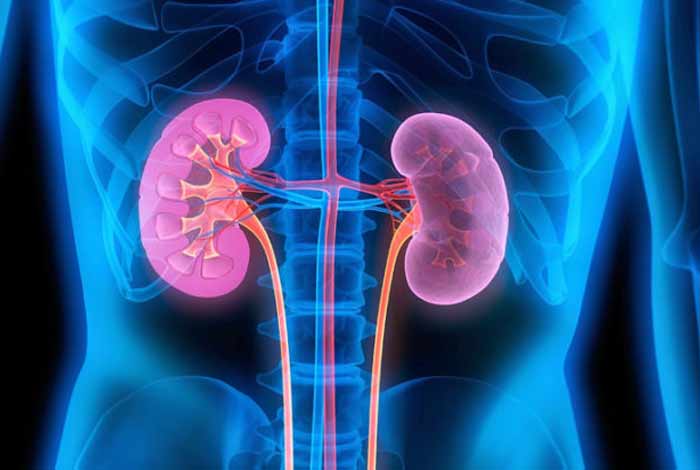
Chronic Kidney Disease (CKD), also known as chronic renal disease, refers to a progressive deterioration of kidney function. Kidneys are two bean-shaped organs, which form an integral part of our renal system. The primary role of kidneys is to flush out waste and toxins from the blood in the form of urine. Kidneys are also responsible for maintaining the fluid and electrolyte balance of the body and regulating the blood pressure. Kidneys release a hormone, called Erythropoietin, which is essential for synthesis of red blood cells in the bone marrow. It also converts vitamin D into its active form, thus maintaining an optimal bone health.
Chronic Kidney disease is marked by a gradual decline in the functioning of kidneys. It is most commonly caused by diabetes and hypertension (high blood pressure).
As per a recent estimate by National Institute of Diabetes, Digestive and Kidney Diseases, approximately 14% of the general population is affected by CKD, with an increased incidence in women (15.93%) than men (13.52%).[1] This justifies the theme for World Kidney Day 2018, led by International Society of Nephrology and International Federation of Kidney Foundations.
Owing to its asymptomatic nature in the initial stages, CKD is also known as “silent disease”. This is the reason, CKD causes more death per year than even the most debilitating cancers, such as breast cancer and prostate cancer.
CKD is a fatal condition and most people die of cardiovascular conditions, like heart attack and stroke. Although CKD has no definitive cure, its progression can be retarded through medications and lifestyle modifications. However, if left untreated, it can further progress to develop into End Stage Renal Disease (ESRD), also known as kidney failure, which would require invasive treatment approaches, including frequent dialysis or kidney transplant.
Symptoms of Chronic Kidney Disease
As already mentioned, CKD does not produce any symptom in its initial stages and patients usually seek medical consultation, after about 25 per cent of kidney damage has already occurred. The presenting complaints of such individuals are as follows.
- Fatigue and low on energy
- Inability to concentrate
- Poor appetite
- Abrupt change in body weight
- Trouble sleeping or Insomnia
- Muscle cramps, mostly at night
- Swelling in feet and ankles (medically termed as edema)
- Puffiness around eyes, particularly in morning
- Dry and itchy skin
- Increased frequency of urination, especially at night but decreased urinary output
- Blood in urine
Other than the commonly encountered presentation, some people may develop other severe symptoms due to complications caused by CKD. These are as follows.
- Anemia
- Chest pain and shortness of breath due to fluid accumulation in lungs (medically known as pulmonary edema)
- High blood pressure (Medically termed as Renal Hypertension)
- Brittle painful bones (Seen in dialysis patients, medically known as Renal Osteodystrophy)
- Inability to achieve or maintain erection in men (medically known as erectile dysfunction)
- Reduced sex drive and Infertility in women and men

Risk Factors of Chronic Kidney Disease
CKD typically occurs in certain high-risk group of people. The major risk factors of CKD are as follows.
- Diabetes: High blood sugar or diabetes is one of the major risk factor associated with CKD. As per an estimate by American Diabetes Association, CKD involves about 23 % of U.S population with diabetes. Uncontrolled type 1 and type 2 diabetes are associated with several complications, such as retinopathy, stroke, neuropathy, cardiovascular diseases, etc. CKD is one of the major complication of diabetes and is termed as Diabetic Kidney Disease. This occurs as the high blood sugar puts excessive strain on kidneys, thus eventually causing kidney damage.
- High Blood Pressure: Hypertension, or an elevated blood pressure, forms another significant risk factor for CKD. For any organ to function efficiently, it must have an adequate blood supply. A persistent high blood pressure can make the blood vessels around the kidney to become narrow, hard or weak. This hampers the blood flow to the kidneys, thus eventually leading to CKD.
Other risk factors associated with CKD are described below.
- Age: CKD mostly affects people in their 60s. It is rarely seen in young age group. Even in the presence of diabetes and hypertension, CKD is seen after a long duration of elevated blood sugar level and high blood pressure. It is not an acute finding and develops slowly over a long period of time, thus presenting itself mostly in elderly individuals.
- Gender: As already stated, women are seen to be affected from CKD more often than men. However, it must be noted that the progression of CKD in women is much slower than in men.
- Ethnic origin: Estimate by National Institute of Diabetes, Digestive and Kidney Diseases, Mexican Americans (15.29%) and African Americans (17.01%) are more prone to develop CKD than Caucasians (13.99%).
- Family History: Presence of a family member or a close relative with a kidney disease puts a person at a higher risk of developing CKD.
- Cardiovascular diseases: Diseases of heart and blood vessels, can seriously impair the blood flow to the kidneys, thus increasing the risk of developing CKD.
- Lifestyle factors: A poor lifestyle, including smoking, alcohol and obesity also predisposes a person to develop CKD.

Do I have Chronic Kidney Disease?
If you have hypertension, diabetes or any cardiovascular condition, you definitely are at risk of developing CKD. If your blood pressure and blood sugar levels are constantly elevated, and you have developed symptoms like changes in appetite, fatigue, weight fluctuations, blood in urine, etc., you may have developed CKD.
Also, if your blood pressure is not coming down to the normal range, you must undergo blood and urine investigations to rule out CKD as kidney plays a vital role in maintaining a normal blood pressure.
Anemia and bone pain along with other risk factors may be suggestive of a deteriorating kidney function.
If you are medically compromised and have a family member with a history of kidney damage or kidney failure, you may develop CKD in the long run or may have reached its initial stage.
Females, in particular of Mexican American or African American origin, who have diabetes or hypertension, and experiencing the above stated symptoms, may have developed CKD.

Causes and Prevention of Chronic Kidney Disease
Causes of Chronic Kidney Disease:
There are a number of causes which can lead to development of CKD, diabetes and hypertension being the leading ones. According to the National Kidney Foundation, about two-third cases of CKD are caused by diabetes and hypertension.[2]
- Diabetes: Uncontrolled high blood sugar can put overdue strain on the kidneys and over a period of time, this can lead to CKD.
- Hypertension: A high blood pressure can severely disrupt the blood flow to the kidneys, thus gradually leading to its damage. An interesting fact here is that, CKD is caused by hypertension and CKD also leads to hypertension. This means that an elevated blood pressure can cause CKD by altering the blood vessels supplying the kidneys. Also, when the kidneys are not functioning normally, the fluid and electrolyte balance of the body is disrupted, which can further increase the blood pressure.
Some of the other conditions which can lead to CKD apart from diabetes and hypertension are:
- Glomerulonephritis: This is one of the most common kidney disease. Glomerulus is the part of kidney which filters waste out of blood and passes it on to the kidney tubules to be finally excreted in urine. When the glomeruli are inflamed, the condition is known as glomerulonephritis. It renders the kidney incapable to filter blood, hence leading to CKD.
- Inherited diseases: Certain inherited diseases can cause damage to the kidneys. One such disease is polycystic kidney disease, which is marked by development of numerous cysts in kidney, which can damage the kidney and the surrounding tissue, thus leading to CKD.
- Congenital renal malformations: These refer to anomalies in the normal kidney structure and/ or function, present at birth. It could be underdeveloped or absence of one or both kidneys. It could be blockage in the renal system, hindering the outflow of urine, thus causing urine to back flow in kidney (medically known as hydronephrosis), causing recurrent infection and eventually causing CKD. Children who frequently acquire UTI (Urinary Tract Infection) may have such blockages.
- Autoimmune diseases: Certain diseases are marked by a hyper-responsive immune system. In these diseases, the immune cells of the body start recognizing its own body cells as foreign infectious agents, thus damaging them. One such disease is Systemic Lupus Erythematosus (SLE) is an autoimmune connective tissue disorder, wherein the immune cells attack its own body organs, including kidney. This can lead to CKD, which in this case is termed as lupus nephritis.
- Obstructions to Urinary Outflow: Presence of a kidney stone, a tumor or an enlarged prostate gland in men can obstruct the outflow of urine, thus leading to CKD.
- Recurrent Urinary Tract Infections: Repeated infection of the urinary tract can gradually damage the kidneys, leading to CKD.
- Prolonged use of certain medications: Some drugs, such as NSAIDs (Non-steroidal Anti-inflammatory Drugs), on prolonged use can damage the kidneys and lead to CKD.
Prevention of Chronic Kidney Disease:
Usually CKD is recognized in its advanced stages, when kidney function has declined considerably. However, taking some precautionary measures can prevent the condition effectively. These measures are as follows.
- Keep your blood sugar in check: Diabetes is one of the greatest risk factor and cause of CKD. Hence, people with type 1 and type 2 diabetes must keep their blood sugar in the normal range, through medications and lifestyle changes. Also, such individuals are recommended to undergo frequent check-ups to diagnose any damage to the kidney in the initial stage itself. This would prevent the onset of severe damage and End Stage Renal Disease, i.e., kidney failure.
- Maintain a normal blood pressure: A high blood pressure is another major cause of CKD. Thus, medical intervention combined with lifestyle modifications can help maintain a normal blood pressure. If you are hypertensive, you must undergo regular medical investigations to recognize and treat kidney damage in its earliest stage.
- Maintain a health BMI: A healthy balanced diet and regular exercise can aid in maintaining a healthy Body Mass Index (BMI). Overweight and obesity predisposes an individual to several medical ailments, such as hypertension, diabetes and other cardiovascular diseases.
- Say No to Smoking and Alcohol: Smoking and alcohol are considered as important risk factors associated with CKD. Hence, abstinence from cigarette smoking and alcohol can lower your risk of developing CKD.
- Take medications judiciously: Unsupervised use of certain medicines, like NSAIDs may cause CKD. Hence, talk to your doctor before taking any medicine and take them only for the duration recommended by your doctor.
Diagnosis and Tests of Chronic Kidney Disease
Diagnosis of Chronic Kidney Disease:
CKD is usually diagnosed as an incidental finding as it usually has no manifestations in its initial stages. However, in its advanced stages, people may seek a medical consultation. CKD can be easily diagnosed by certain diagnostic investigations, which are described below.
- History of Symptoms: Your doctor will take a detailed history of the symptoms you have been experiencing. The most important part of the patient’s history in CKD is medical history. Your doctor will seek information of medical ailments, in particular diabetes, hypertension and other cardiovascular diseases. Your doctor will also ask if any of your family member has a history of CKD or kidney failure. After a thorough history, your doctor may order some blood and urine investigations if suspecting CKD.
- Blood tests: Glomerular Filtration Rate (GFR) is one of the definitive indicator of kidney function. GFR refers to the rate at which the kidney filters waste and toxins out of your blood. Normally, it is about 120 mL/ minute. In CKD, the inability of kidneys to filter blood will present itself as a low GFR. A low filtration rate will cause accumulation of waste products and toxins in the blood. Creatinine and urea are most significant waste products that are retained in the blood in CKD. The levels of creatinine in blood is used to measure the GFR. Assessment of GFR helps the doctor in evaluating the stage of CKD. A high blood creatinine level is suggestive of a low GFR and is a reliable indicator of CKD. The level of urea is tested by a specific blood test, known as Blood Urea Nitrogen (BUN).
- Urine tests: Individuals with adequately functioning kidney usually do not excrete blood and protein in urine. However, a deteriorating kidney function in CKD will show presence of blood (hematuria) or protein (proteinuria) in urine.
- Imaging Tests: Although blood and urine tests constitute the main investigations to diagnose CKD, your doctor may also order ultrasound or CT scan of your kidney. This assists in determining specific anomaly in the renal system, including size and shape of kidney, presence of any blockage in the kidney or urinary tract, assessing the blood flow to the kidneys and check for presence of any tumor or kidney stone.
- Biopsy: In some cases, doctor may order a biopsy of your kidney tissue to determine the factor causing kidney disease. Biopsy refers to removing a small section of kidney tissue, under the effect of anesthesia and sending the removed tissue to the lab for microscopic evaluation.
Stages of CKD
After appropriate investigations have been carried out, a nephrologist determines the stage of Chronic Kidney Disease. The various stages are described below.
Stage 1: Kidney damage, but function of kidney is normal (estimated GFR is more than or equal to 90 mL/ min) and there is persistent proteinuria (for more than or almost 3 months)
Stage 2: Kidney damage with a mild disruption of kidney function (estimated GFR lies between 60 to 90 mL/ min) and there is persistent proteinuria (for more than or almost 3 months).
Stage 3: There is a mild to severe loss of kidney function (estimated GFR is 30 to 59 mL/ min)
Stage 4: There is severe loss of kidney function (estimated GFR is 15 to 29 mL/ min)
Stage 5: End Stage Renal Disease (ESRD) or kidney failure (estimated GFR is less than 15 mL/ min) and patient cannot survive without dialysis or transplant

Treatment and Care of Chronic Kidney Disease
Treatment of Chronic Kidney Disease:
There is no cure to reverse the damage caused in CKD. However, if left untreated, the disease may progress to the stage of kidney failure. Hence, several treatment methods can be advocated to arrest the damage caused to the kidneys. These treatment methods are described below.
1. Treat the underlying cause: It is a well-known fact that diabetes, hypertension and cardiovascular diseases are the major causes of CKD. Hence, consult a medical professional to receive appropriate treatment for these health conditions. Various drugs used to treat type 1 and type 2 diabetes include glimepiride, metformin, insulin, etc. Drugs for hypertension include Angiotensin converting enzyme (ACE) inhibitors, diuretics, etc. Once the blood sugar level and blood pressure are controlled, the progression of CKD can be arrested. Regular monitoring is needed to evaluate the blood pressure and blood glucose levels.
2. Treatment of anemia: Kidneys form a hormone, called erythropoietin, which is needed to form red blood cells. Hence, CKD can cause anemia. This can be treated by erythropoietin supplements, occasionally with added iron. Treating anemia also relieves fatigue seen in CKD.
3. Treatment of swelling: The swelling of feet and ankles seen in CKD occurs due to fluid retention in the body. This can be treated by drugs, such as diuretics, which restore the fluid balance of the body, thus relieving swelling.
4. Medications to protect bones: Kidneys convert the vitamin D into its active form. This active form is needed to maintain normal calcium and phosphate levels in blood. Vitamin D is needed to absorb calcium from the food we eat. Hence, CKD can cause weakening of bones, making them susceptible to fracture. It is treated through vitamin D and calcium supplementation. Phosphate binder, such as calcium carbonate is another group of drugs which is given to prevent an increase in phosphate levels of blood.
5. Medications to manage cholesterol levels: People with CKD are at a high risk of developing high cholesterol levels. This is the reason that most patients of CKD die due to a heart attack. Hence, CKD patients are asked to take drugs, such as statins to prevent this complication. Regular monitoring of serum cholesterol level is recommended.
Some patients may report to the doctor with a highly progressed kidney damage, known as End Stage Renal Disease. This is also known as kidney failure and cannot be managed solely through medications and lifestyle changes. The treatment of ESRD involves dialysis and kidney transplant. These are described below.
- Dialysis: When the kidneys are unable to filter waste out of blood, it can be done with the aid of machinery and catheters. This process of filtering blood artificially is referred to as dialysis. It is of two types, namely hemodialysis and peritoneal dialysis. In hemodialysis, the blood continuously enters a machine, which filters the blood of the patient. In peritoneal dialysis, the dialysis solution is infused in the abdominal cavity of the patient with the help of a catheter. The solution along with the waste is then drained out.
- Kidney Transplant: This is usually done in severe cases, when kidney functioning has absolutely declined. Kidney transplant is a surgical procedure which involves replacing the damaged kidney of the patient with a healthy kidney, taken from a donor. Donor is preferably a parent or a sibling. Patient may need to be on medications life-long to prevent rejection of the transplanted kidney by the patient’s body.
However, it must be noted that dialysis and kidney transplant are invasive procedures and have numerous side-effects associated with them. Hence, these are used only in cases which are severe enough to offer a low life-expectancy with other treatment approaches.
Care for People with Chronic Kidney Disease
Chronic Kidney Disease can render an individual physically and mentally weak. It affects all aspects of patient’s life. Hence, leading a normal life may be difficult for such individuals. Family members, friends and peers must provide appropriate support to the patient.
Encourage the patient to adopt a healthy lifestyle, including a healthy diet, regular exercise and abstinence from smoking and alcohol.
Make sure the patient is taking the medications on time and is attending follow-up appointment with the doctor regularly. A regular monitoring of patient’s blood pressure, blood sugar levels and cholesterol level is of paramount importance in CKD patients.
Deficiency of vitamin D and calcium can cause skeletal discomfort to the patients, making their day-to-day chores difficult. Hence, family and peers must assist them physically and provide them emotional support.

OTC or Self-Management Methods for Chronic Kidney Disease
OTC for Chronic Kidney Disease:
Some over-the-counter medications are available to treat few symptoms of CKD. These include supplements of iron, vitamin D and calcium. Phosphate binder, such as calcium carbonate is also available over-the-counter.

Self- Management Methods Available
Although medications form the mainstay of treatment of CKD, without certain dietary and lifestyle modifications, no treatment can be effective. The self-management methods for CKD are as follows.
1. Dietary modifications
Since kidney is the primary organ concerned with regulating fluid and electrolyte balance, dietary changes form an integral part of any kidney disease. American Kidney Fund suggests the following dietary changes to produce a “kidney-friendly diet”.[3]
- Restrict salt intake in diet- Salt is a rich source of sodium. Excessive salt intake can worsen the high blood pressure, thus further affecting kidneys. Also, salt is known to retain fluid in the body. Since, CKD is already marked by excessive fluid retention, increased salt intake can further aggravate the condition. Hence, restrict salt intake in your diet. Avoid foods with added salt such as frozen food items, canned soup, processed meats, etc.
- Limit your potassium intake- Potassium is needed to maintain the health of the muscles. However, CKD may cause an imbalance in the potassium levels. Hence, low-potassium diet should be consumed. These include apple, cranberries, cauliflower, white bread, white rice, etc. Avoid avocados, banana, spinach, beans, etc. as they are rich in potassium.
- Reduce phosphorus in your diet- Phosphorus along with vitamin D and calcium, is necessary for maintaining bone health. Chronic Kidney Disease can cause an increase in phosphorus levels in the blood. Thus, it is important to reduce your daily phosphorus intake. Your dietitian may ask you to consume corn or rice cereal, Italian bread, etc. as they are low in phosphorus. Avoid phosphorus-rich foods, such as whole-grain bread, nuts, oatmeal, sunflower seeds, etc.
- Limit your fluid intake- Since CKD causes excess fluid to stay in your body, instead of getting flushed out, excess fluid intake can worsen the condition. Use small cups to consume less fluid. Excess salt can also increase thirst, hence must be avoided. Chewing gums and candies can reduce your thirst. Choose sugar-free gums if you have diabetes.
- Limit protein in your diet- In CKD, kidneys are incapable of filtering blood effectively. An increased protein in diet can further strain the kidney, thus worsening the kidney damage. Hence, a dietitian should be consulted to estimate the grams of protein you need per day, so as to avoid excess protein intake.
2. Weight Management
Overweight and obesity in a CKD patient can further elevate the blood sugar levels and blood pressure, thus worsening the health of the kidney. Also, CKD increases the risk of elevated cholesterol in blood. Hence, regular physical activity can play a great role in managing weight and thus, arresting the progression of CKD.

Natural Ways to Cure Chronic Kidney Disease
Along with conventional medicine, alternative medicine is pacing up to effectively treat Chronic Kidney Disease. The several natural ways to manage CKD are as follows.
- Yoga: Research has shown a direct relation of oxidative stress with CKD. It also validated the role of yoga in reducing this oxidative stress. It was seen that 30 minutes of yoga for 4 months significantly reduced oxidative stress and produced dramatic results in patients of CKD. Certain asanas such as Ardha chakrasana (backward bending from waist), Shashankasana (Hare pose) and Supta svastikasana (reclining cross-legged posture) have been shown to benefit in CKD.[4]
- Tai chi: Recent study has shown that a Chinese martial art, called tai chi improves the lipid metabolism and thus, improves the blood flow to kidneys. Hence, tai chi can effectively counteract CKD.[5]
- Acupuncture: It is a component of traditional Chinese medicine, which involves inserting fine needles in certain points of the body. Research has shown that acupuncture can improve the GFR and reduce the blood creatinine levels in CKD.[6]
- Infrared therapy: This therapy involves exposing the concerned area to infrared light, which can penetrate into the deeper tissues. Research has shown that infrared therapy on certain acupoints, for 30 minutes, for three times a week for two months significantly reduced the blood urea and creatinine levels. Hence, it has been proven to be effective in CKD.[7]

Health Tips by Experts
According to Experts, each individual with hypertension, diabetes and other cardiovascular condition lies in the high-risk category of Chronic Kidney Disease. Hence, a regular monitoring of Kidney functioning is vital to avoid kidney disease. The importance of maintaining a normal blood sugar level and a normal blood pressure must be realized by such individuals.
However, if you have been diagnosed with CKD, do not lose hope as the disease can be arrested at this stage itself through medical help and lifestyle changes. Keep yourself motivated to lead a healthy life.