Tuberculosis – World’s Deadliest Infection alongside AIDS

Introduction
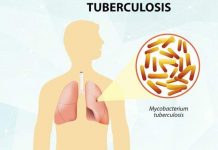
Tuberculosis (TB) is a bacterial disease caused by Mycobacterium tuberculosis, which has been present on the earth for nearly 15,000 years. Humans have shared a long-running, dysfunctional relationship with the deadliest disease, which can be traced back to 2400-3400 BC when Egyptians used to mummify their dead. Signs of TB have been discovered in the spinal cord of some of these mummies. There are two theories regarding how TB originated. One of the theory postulates that the bacterium responsible for causing TB originated in domesticated animals and then it passed on to humans. While the other theory points to the fact that this disease originated with early humans themselves and had nothing to do with animals. It spread to the world as the human population grew and migrated. TB can be accounted as the deadliest gift to the world population from Africa, along with HIV/AIDS, which also has its roots in the same continent.
Tuberculosis or TB has been referred to as Pott’s disease, scrofula, phthisis, consumption and the white plague over its entire course in the human history. Dr. Robert Koch created history by discovering the bacterium that caused ‘Captain of all these men of Death’ or tuberculosis. This discovery was a milestone in controlling this deadly disease which killed one out of every seven people residing in Europe and the U.S.A. at that time. A century later, in order to mark the importance of this day in the history of mankind and to raise awareness among the people about this disease, March 24 was designated as World TB Day. World TB Day will not be a true celebration until this deadly disease becomes a thing of past.
Tuberculosis is the number one global killer in the infectious disease category, affecting nearly1/3rd of the world population but there are a number of misconceptions among the people regarding this disease. In Europe, people believe that this deadly disease is already extinct. Much better response and preparedness was observed in people living in North America.
Active tuberculosis is known to have close ties with poverty and people living in low- and middle- income group countries are the most common victims. However, vulnerable and marginalized populations like refugees, migrants, elderlies, drug users and alcoholics living in high-income group countries are also an easy prey to this disease.
The reason TB has stuck with humans for such a long time is because of a mutation that occurred in the DNA of this bacterium that allowed it to go dormant in its hosts and appear again decades later. It emerged as a survival strategy for the bacterium and gave it the opportunity to spread in the otherwise scattered human settlements in the earlier days.
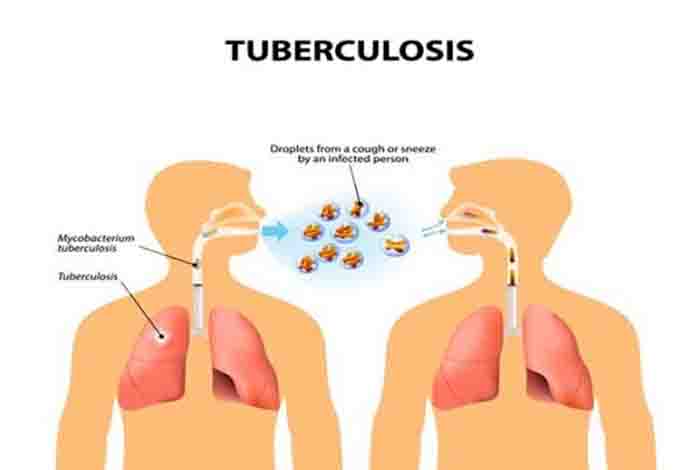
Transmission of TB
TB is an airborne disease in which the bacteria are carried in airborne particles, known as droplets, that are 1-5 micrometer in diameter. They are generated when a person who has TB in the lungs coughs, shouts, spits, sneezes or sings. These droplets can remain suspended in the air for a long period of time, depending on the climate. However, it should be noted that the disease only spreads through air contact and not surface contact. When these droplets are inhaled by a healthy person, the bacteria enter the body and reaches the lungs through the respiratory system passageway.
After entering the body, the disease is known to undergo three stages, primary infection, latent infection and active disease. Primary TB infection refers to the infection occurring in the lungs after being exposed to the bacteria. Most of the people recover from it. Latent infection occurs when the person shows no signs of the disease and is non-infective. The bacterium is said to in dormant stage at this point. Since TB is known to be an opportunistic infection (OI), the disease develops into an active phase in people who have weakened immune system due to old age, malnutrition, immunosuppressant drugs and HIV infection. HIV stands for human immunodeficiency virus, which as its names suggest, weakens the immune system of its host, making it more susceptible to infections. With time, HIV causes extensive damage to the immune system and eventually leads to the development of acquired immunodeficiency syndrome (AIDS) in the host.
Tuberculosis and AIDS
Tuberculosis and HIV have gone hand in hand since AIDS emerged on the face of the earth. It is common for the people with HIV infection to get TB because of the weakened immune system. The infection with both HIV and TB is known as HIV/TB co-infection. [1] Latent TB is more likely to advance into active TB in people with HIV infection. Furthermore, TB is known to worsen the condition of HIV patients. The contribution of HIV in increasing the global prevalence of TB is huge. Although, HIV related TB is both preventable and curable, the incidence of co-infection keeps on climbing the ladder in developing countries where HIV and TB, both are rampant and limited treatment options are available. Toxicities arising from medicines used for treating HIV and TB overlap, they interact and the immune reconstitution inflammatory syndrome (IRIS) make the treatment of HIV/TB co-infection extremely difficult.
Globally, the leading cause of death in HIV patients is TB. In countries where HIV medicines are more readily available, lesser people die from TB, because these medicines decrease the person’s susceptibility to acquire TB and decrease the chances of latent TB to develop into active disease. If prompt treatment is not given, TB can very quickly progress from disease to death in HIV patients. TB is known to kill 1 out of every 3 AIDS patients. [2]
Global TB/HIV Co-Infection Statistics
WHO estimates that globally, nearly 14.8% of people with TB have HIV co-infection. In sub-Saharan Africa, the percentage of HIV/TB co-infection is as high as 50-80%. Between 1985 and 1990, there was a 20% upsurge in the number of TB cases being reported, which accounted for nearly 28,040 more cases. Out of these extra cases, nearly 30% were AIDS-related TB, as estimated by The U.S. Centers for Disease Control and Prevention (CDC). [3]
By 1992, the percentage of TB started declining in the U.S and by 2010, it was brought down to a rate of 3.6 cases per 100,000 people, the lowest rate till date. [4]
According to WHO, in 2016 deaths from HIV/TB co-infection tallied to 374,000 globally. Deaths of these people are reported to have occurred from HIV. The total number of people who died from HIV infection is estimated to be around 1.2 million. Therefore, the number of people who died from HIV infection alone is 826,000. People who lost their lives to TB infection alone is estimated to be 1,300,000. Therefore, TB is a bigger killer than HIV/AIDS. Nearly 10% of the people who have TB are known to be HIV positive.
| Region | Total Mortality | 0-14 years TB mortality | Male>15 years | Female >15 years | Population |
| Africa | 320,000 | 43,000 | 177,000 | 100,000 | 989,000,000 |
| Americas | 6,200 | 1,860 | 2,900 | 1,500 | 991,000,000 |
| Eastern Mediterranean | 3,000 | 470 | 1,400 | 1,100 | 648,000,000 |
| Europe | 5,100 | 860 | 3,000 | 1,200 | 910,000,000 |
| South-East Asia | 35,000 | 2,600 | 20,000 | 9,900 | 1,930,000,000 |
| Western Pacific | 5,000 | 1,710 | 2,200 | 1,000 | 1,860,000,000 |
| Global Total | 374,000 | 52,000 | 207,000 | 115,000 | 7,320,000,000 |
Table1: Estimated WHO TB mortality statistics for HIV positive people in 2016 by age and region
The African region of WHO alone accounted for 86% of the deaths from HIV/TB co-infection, with male: female ratio being 1:8. In the Eastern Mediterranean regions of WHO, male: female ratio of mortality due to co-infection was found to be 1:3 and 2:4 in the European region of WHO. African region carries the world’s burden of HIV/TB co-infection, where a whopping 81% of TB patients tested positive for HIV. [5]
Impact of HIV Infection on the pathogenesis of Tuberculosis
When a person inhales the M. tuberculosis loaded air droplets, it goes into the alveolar sac of the lungs, where it is engulfed by the macrophages, which form the first line of defense. The bacteria which survive multiply within the macrophage and are spread to other areas of the body. In HIV patients, the macrophages are defective and are unable to provide the necessary protection. They might even increase the person’s susceptibility to TB. However, there is no conclusive evidence supporting the fact that HIV infected people are more susceptible to TB than healthy people, on the same level of exposure. [6]
Symptoms of TB in people with HIV
Classic symptoms of pulmonary TB might or might not be observed in HIV positive people. Some of these patients have fewer symptoms of TB or, they are not specific. On top of that, some of these patients have normal chest X-rays. Patients who are HIV positive and have TB co-infection might frequently develop sub-clinical TB, which is not identified as TB and therefore there is a delay in accurate diagnosis and treatment of TB.
People with HIV infection are at a higher risk of developing extra-pulmonary TB as compared to people without co-morbidity. Statistically speaking, 40-80% of HIV positive people with TB develop extra-pulmonary disease in comparison to 10-20% of TB patients without HIV.
Extra-pulmonary TB occurs when M. tuberculosis infects other organs and tissues of the body, apart from lungs, like pleura, abdomen, bones and joints, spinal cord, lymph nodes and the brain and its coverings. On rare occasions, other pathogens, called atypical mycobacteria or Non-Tuberculous Mycobacteria can also result in illnesses that mimic the symptoms of TB. For example, Mycobacterium bovis is reported to cause tuberculosis of abdomen in some people after drinking raw milk.
The Stigma of TB and HIV/AIDS
In the earlier days of HIV/AIDS epidemic, when people died of AIDS, they were reported to have died from TB infection rather than AIDS. Otherwise, the family of the deceased would be out-casted from the society. Even today, when medical science has made tremendous progress in finding a cure for these lethal diseases, patients still face discriminations at every level of society. Having TB is supposed to send a hidden signal that the patient actually has HIV infection. Therefore today, in order to protect the patients from further mental agonies, the actual identities of the people having TB and HIV are kept a secret.
Conclusion
Although the advancements in medical science have helped in saving nearly 53 million lives since 2000, TB still remains a major public health issue in the world. WHO has been on its toes on gathering and analyzing data about the trends of TB outbreak for determining ways to eradicate it. A number of control programs are being run by WHO throughout the world to help the nations crippled by TB. When efforts do not bear fruits and TB continues to claim more than 4000 lives each day, people start to lose hope.
The HIV/TB co-infection demands a special attention as it is the number one killer of HIV patients. Even though the world has pledged to eradicate TB by 2030, the efforts do not match the magnanimity of the situation. With each passing minute, it demands more commitment and more resources. The need of the hour is to adopt a more dynamic, multi-sectoral and global approach.